-
High-speed rail project, rent controls: Toulouse candidates divided for municipal election
Tight race expected in city as far left home in on quarter of vote share
-
Travelling from France to UK: dual nationals warn over passport renewal issues
It comes as the UK enforces its electronic travel authorisation (ETA) scheme
-
‘If I lower the price I close’: fuel station manager in western France defends €2.97 diesel price
The small station in Deux-Sèvres is selling the most expensive diesel in the country amid the ongoing fuel price spike
Why have some people still not had Covid? French study asks
The report considered a variety of factors from genetic mutations to blood type to lifestyle choices
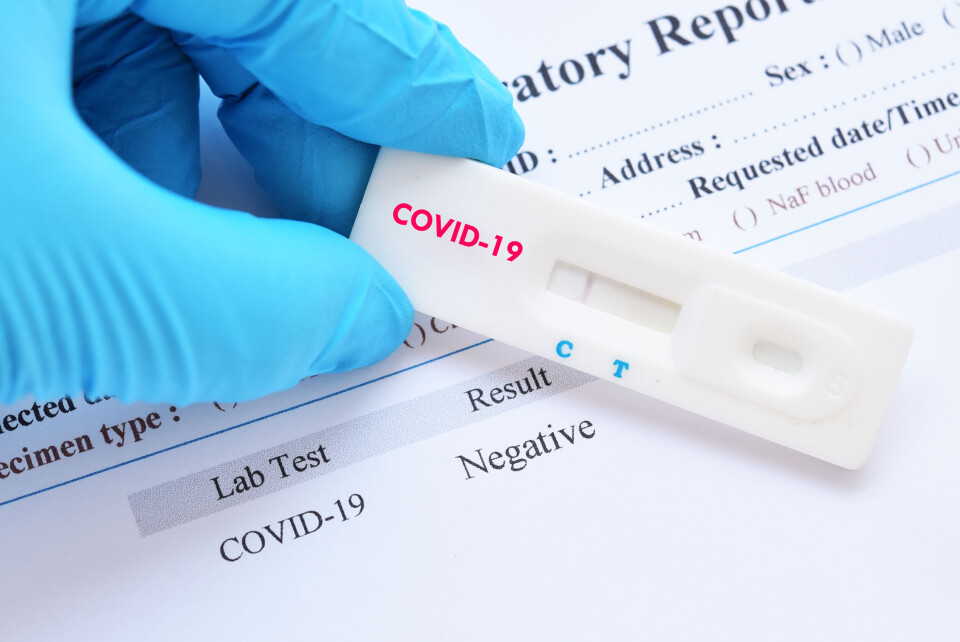
An international study led by a French professor has explored why some people escaped Covid infection (or had only very mild symptoms), even early on in the pandemic or when working in high-risk spaces.
The report recruited 300 people who appeared resistant to the Covid virus infection, and considered a variety of factors, from genetic mutations to blood type, to interaction with other viruses, to lifestyle.
It looked at people who seemed to have escaped the virus or had only very mild symptoms, even if their work put them at high risk, and even before measures such as mask-wearing were introduced.
Professor Laurent Abel, co-director of the laboratory of human genetics of infectious diseases at the Imagine institute, Inserm, at the Necker Hospital in Paris, was one of the leaders of the study, alongside Jean-Laurent Casanova, at the Rockefeller University in New York.
Professor Abel told Le Monde: “The typical example is that of close intra-family exposure. In a couple, for example, one of the two partners may be affected without always being aware of it: the other partner may remain unaffected.
“What we are studying are mutations that reduce the risk of infection by at least a factor of 10.”
In the study, which has been published in the scientific journal Nature Immunology, the authors wrote: “The proportion of humans with natural resistance to infection by SARS-CoV-2 is unknown. [But] a certain number of genetic causes were suggested.”
The authors said they ascertained the absence of infection through negative PCR tests and a subsequent negative blood test for antibodies.
Professor Olivier Schwartz, head of the virus and immunity unit at the Institut Pasteur in Paris, explained that there are “three types of protective factors that can be combined: genetic, immunological and environmental”.
Genetics
The study considered the genomes of apparently-resistant people, in a bid to track rare mutations of certain genes, which could potentially offer protection.
Etienne Decroly, a virologist at the CNRS at the University of Aix-Marseille, said: “If innate immunity detects the virus quickly, it will limit the impact of the infection.
“On the other hand, if the immune system detects it too late, viral loads can reach high levels, leading to a risk of the immune system going into overdrive, which can lead to severe forms of the disease.”
Professor Jean-Daniel Lelièvre, head of the clinical immunology and infectious diseases department at Henri-Mondor Hospital in Créteil (AP-HP), explained: “It’s not black and white, it is more like 50 shades of grey.”
Yet, he believes that several “genetic variants” are likely involved in the susceptibility to the virus.
Blood type
Blood type is also being considered: an earlier meta-analysis of 46 studies on the subject across almost 50,000 people found that, for example, the O blood type may “offer a very modest protective effect” of around 10%.
Dr Laurent Bardiaux, director of the Etablissement français du sang (EFS) Occitanie, told La Dépêche: “Since the start of the Covid-19 pandemic, at least 40 studies have been conducted on the question of contamination according to blood type. They show that there may be a lesser impact of SARS-CoV-2 according to blood type.”
In France, 42% of people are group O, 44% group A, 10% group B and 4% group AB.
By this measure, people of group O are statistically protected from the other 58% who could transmit the virus to them. But these are only hypotheses.
Dr Nardiaux added: “Beware, the studies we are talking about were carried out before the arrival of the Omicron variant, and some even before Delta.”
Lifestyle
Lifestyle factors are also being evaluated. During the first wave of Covid, scientists found that tobacco smoking could offer a protective effect.
Mahmoud Zureik, professor of Epidemiology and Public Health at the University of Versailles-Saint-Quentin (Yvelines), said: “Nicotine appears to interact with the ACE2 receptors, stopping the virus from entering into cells.”
However, he said that “this requires confirmation, and even if it were confirmed, it’s an impossible message to send, given the disastrous effects of tobacco on health”.
Read more:French study: Nicotine may protect against Covid-19
Similarly, in April 2020, the World Health Organisation confirmed that smokers actually “risk getting a more severe form of Covid than non-smokers”, given that smoking itself reduces lung function, which plays more of a role than any possible protective effect of nicotine.
Virus exposure
The study also considered whether some people were genetically immune to the new coronavirus due to historic exposure to a virus in the same family.
A study published in the scientific journal Nature Communications in January, led by Imperial College London, found that of 52 people who were living with someone who had contracted Covid, 26 had not been infected with it themselves.
These people were dubbed the “immune elite” and had T cells (fighter cells) from exposure to other similar viruses, such as those that can cause colds.
Virologist Mr Decroly said: “This cellular immunity is robust, and is less susceptible to mutations in the spike protein on the [Covid] virus surface.”
However, this immunity only lasts a few months. Yet, this protective effect was seen as encouraging, given the frequency of seasonal colds.
Professor Schwartz said: “We still need to ascertain what is the real level of protection against Covid conferred by these T cells.” More studies with more data are required, he said.
The genetic study is similar in concept to those conducted in the 1990s, on people who were resistant to the HIV virus despite being at risk. The studies found that a rare mutation of the CCR5 gene, which controls the production of cell proteins, offers a protective effect against the virus.
The mutation is likely very rare, however, explained Prof Lelièvre. He said: “Less than 1% of the population have the [CCR5] mutation.”
Related articles
French study: 20% severe Covid patients have genetic or immune issue
New French study reveals places where Covid infections most likely
























